Overview
The glenohumeral joint is a ball (the humeral head) and a shallow socket (the glenoid). When cartilage wears through from osteoarthritis or inflammatory arthritis, the joint grinds and motion becomes painfully limited. An anatomic total shoulder replacement resurfaces the ball and socket with a metal-on-polyethylene articulation — restoring a smooth glide — but only works if the rotator cuff is intact to keep the replaced ball centered.
How the Procedure Works
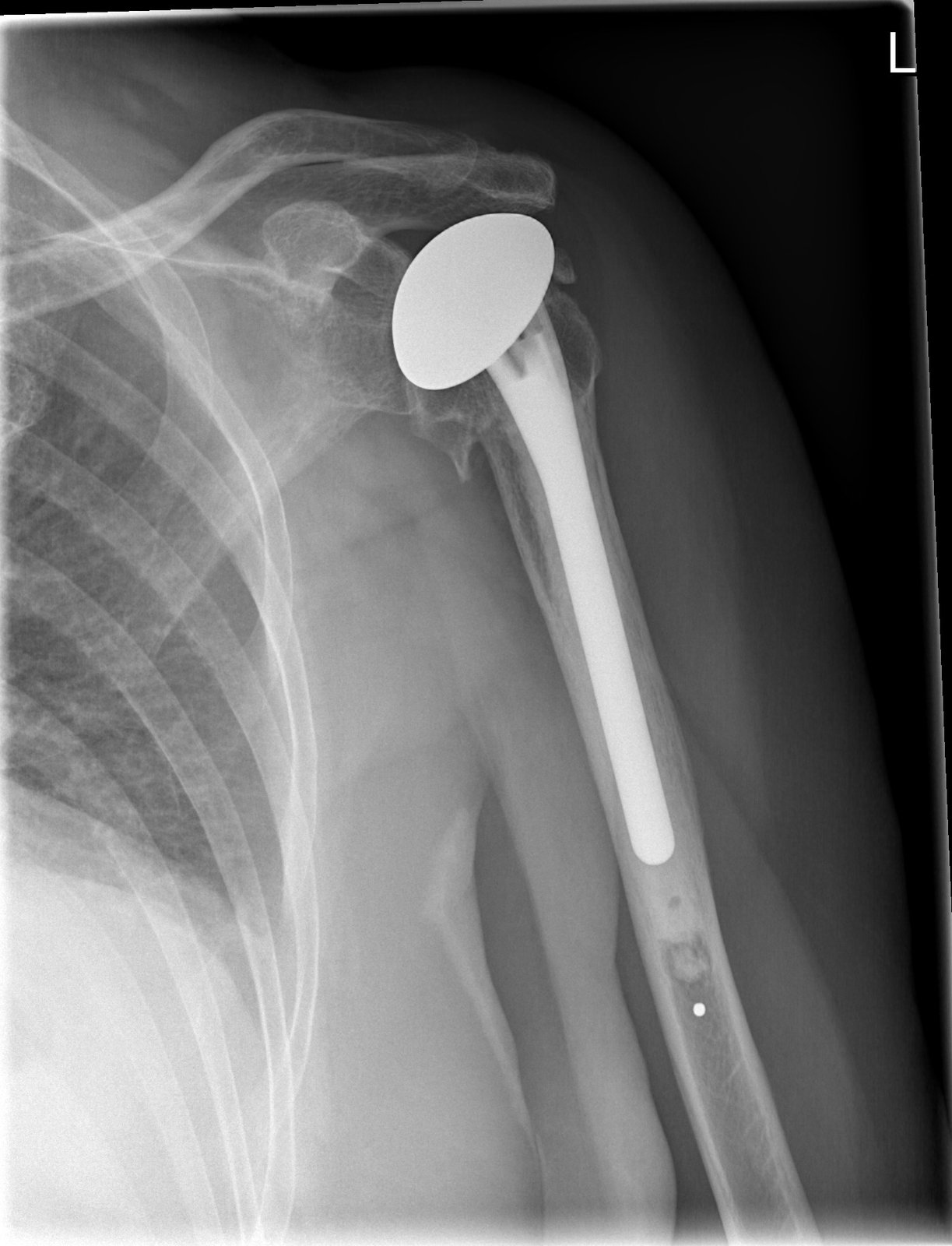
We approach through the deltopectoral interval and take down the subscapularis carefully — it must be repaired securely at the end, because subscapularis failure is a leading cause of instability after anatomic shoulder replacement. The humeral head is cut at the anatomic neck angle, a metal head-and-stem implant is seated, and the glenoid is prepared for a polyethylene socket. Glenoid component positioning is the most technically demanding part: even a few degrees of version error changes how the humeral head loads the socket and accelerates wear. We size the humeral head to restore the native offset and tension the soft tissues evenly — check internal and external rotation, confirm the subscapularis repair is tight, then close. The rotator cuff and deltoid do exactly what they did before surgery; the implant simply gives them a smooth surface to work against.
When to Consider Total Shoulder Replacement
Total shoulder replacement is generally offered when symptoms, imaging, and a trial of non-operative care together point to surgery as the next step. The typical picture includes:
Advanced glenohumeral arthritis
Radiographic bone-on-bone arthritis with matching pain and motion loss.
Intact rotator cuff
A functioning cuff is a prerequisite for an anatomic replacement to succeed.
Exhausted non-operative care
Failed response to activity modification, NSAIDs, therapy, and intra-articular injections.
Conditions This Treats
Physicians Who Perform Total Shoulder Replacement
David B. Templin, M.D.
Trent Twitero, M.D.
Providers Who Surgically Assist with Total Shoulder Replacement
Sydney Georg, PA-C
Ben Swanner, PA-C
Further Reading
External patient-education references and related OSI pages for additional background:





