Overview
what it is and why it matters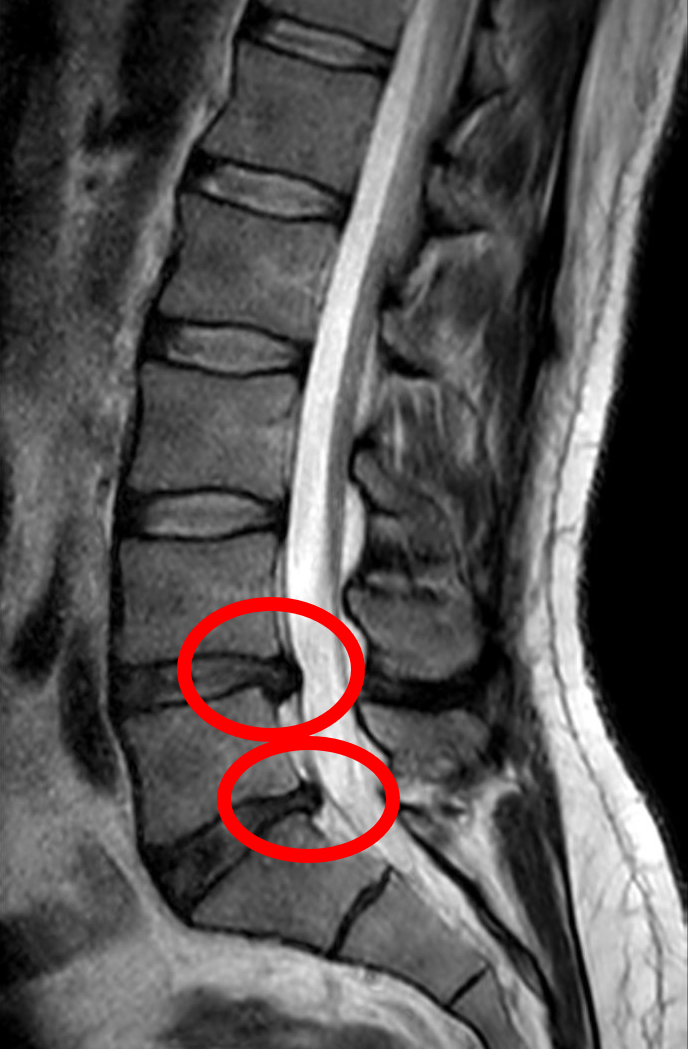
A lumbar disc herniation is the most common cause of pain that travels down the leg — what most patients know as sciatica. Each disc between the vertebrae of the lower spine has a soft gelatinous center, the nucleus pulposus, encased in a tougher outer ring, the annulus fibrosus. When the outer ring tears or weakens, the inner core can push backward into the spinal canal and press against one of the nerve roots that exits at that level. The nerve root becomes irritated both by the mechanical pressure and by inflammatory chemicals released from the disc itself, producing pain that follows the nerve's path rather than staying in the back.
The levels most often affected are L4-L5 and L5-S1, which compress the L5 and S1 nerve roots — the nerves that feed the front and back of the leg down to the foot. Symptoms are classically worse with sitting, bending, and anything that raises pressure in the abdomen (a sneeze, a cough, straining on the toilet), because those movements push the herniated material harder against the nerve. The large majority of lumbar disc herniations resolve with nonoperative care as the displaced fragment shrinks and inflammation subsides — surgery is the exception, not the rule.
Diagnosis
exam first, imaging secondStraight leg raise (SLR) test — leg pain reproduced at 30–70° — is sensitive for L4-5 and L5-S1 herniations. MRI is the standard imaging test. The presence and location of herniation must correlate with clinical symptoms (MRI-positive findings are common in asymptomatic adults).
Treatment Path
how care progresses at OSIActivity modification
Avoiding prolonged sitting and positions that worsen leg pain. Continued walking is encouraged.
Physical therapy
McKenzie extension exercises, core stabilization, and neural mobilization.
NSAIDs / short-term oral steroids
Reduce nerve root inflammation.
Lumbar epidural steroid injection (ESI)
Transforaminal or interlaminar ESI delivers corticosteroid directly to the inflamed nerve root, providing significant relief in 70–80% of patients and often avoiding surgery.
If Surgery Is Truly Needed
rare for most patientsMost lumbar disc herniations resolve with a structured non-operative plan. Surgery becomes the right step for a small number of patients — typically those whose leg pain, weakness, or numbness has not improved after a genuine trial of care, or patients with red-flag findings such as progressive motor weakness or cauda equina syndrome (loss of bowel or bladder control), which is a medical emergency. When surgery is indicated, OSI coordinates it: imaging, records, and scheduling are handled for you.
Emergency. Bilateral leg weakness, saddle numbness, or loss of bladder or bowel control is a surgical emergency — go to the nearest emergency department rather than waiting for a clinic appointment.
Further Reading
authoritative sourcesExternal patient-education references and related OSI pages for additional background:
