Overview
what it is and why it matters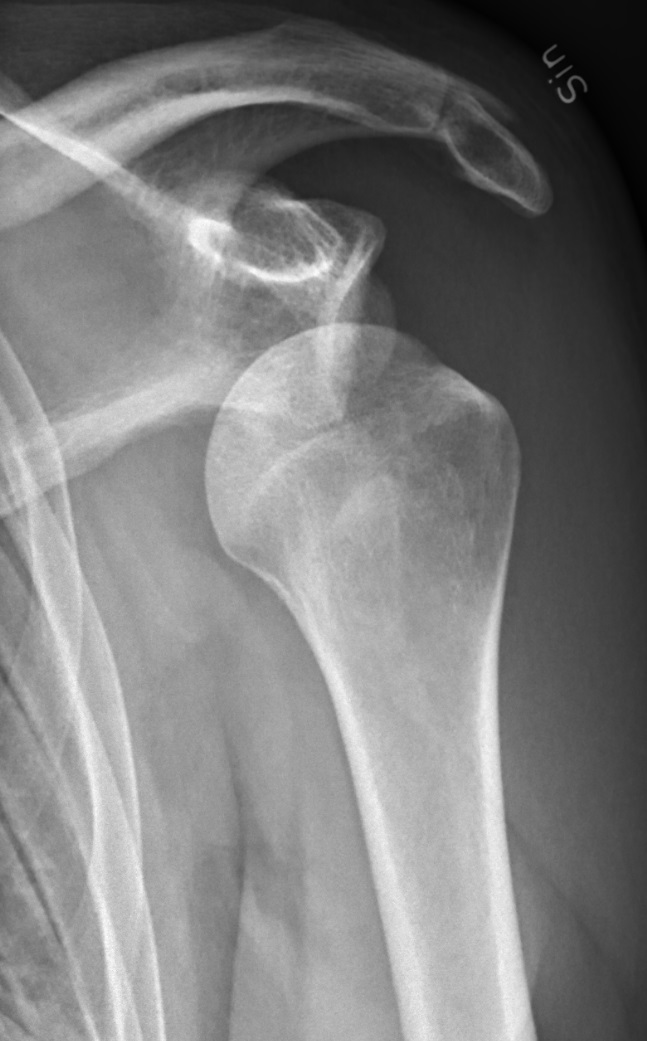
The shoulder is the most commonly dislocated joint in the body, and it pays for its remarkable range of motion with a correspondingly loose fit. The head of the humerus (the ball) sits against a shallow, almost flat surface on the scapula called the glenoid (the socket), held in place largely by soft-tissue restraints — the labrum that deepens the socket, the joint capsule, and the surrounding rotator cuff tendons. When a force drives the arm backward and outward, as in a tackle or a fall with an outstretched arm, those soft-tissue restraints give way and the ball slides forward out of the socket. Nearly all dislocations (around 95%) go in this anterior direction; the less common posterior dislocation is classically caused by a seizure, an electric shock, or a heavy eccentric load.
The first dislocation almost always does lasting damage to the structures that hold the joint together. The labrum and anterior capsule often tear off the front rim of the socket — a Bankart lesion — and the back of the humeral head can dent where it impacted the rim of the glenoid on the way out. Once the soft-tissue restraints are stretched or torn, the shoulder is at real risk of dislocating again, and the probability is highest in younger patients with the greatest number of future years at risk. This is why a first shoulder dislocation is not just an event to be reduced and forgotten — it is the beginning of a stability problem that has to be managed.
Diagnosis
exam first, imaging secondAcute severe shoulder pain with the arm held in a guarded position. Anterior dislocation: the shoulder looks squared-off with a palpable void under the acromion. Neurovascular exam for axillary nerve injury (patch of numbness over the lateral deltoid) is essential before and after reduction. Post-reduction X-rays (AP, axillary, scapular Y) confirm reduction and identify associated fractures.
Treatment Path
how care progresses at OSIClosed reduction
Performed in the emergency setting with procedural sedation or analgesia using any of several reliable techniques (Cunningham, Stimson, traction-countertraction). Post-reduction sling for 1–4 weeks.
Physical therapy
Rotator cuff and periscapular strengthening to reduce recurrence risk after a first dislocation.
Surgical Options at OSI
if non-operative care isn't enoughRecurrent dislocation, first-time dislocation in a young contact athlete, associated fractures requiring fixation, and significant bone loss are indications for surgical stabilization.
Providers Who Treat Shoulder Dislocation
sports-medicine teamDavid B. Templin, M.D.
Trent Twitero, M.D.
Further Reading
authoritative sourcesExternal patient-education references and related OSI pages for additional background:



