Overview
what it is and why it matters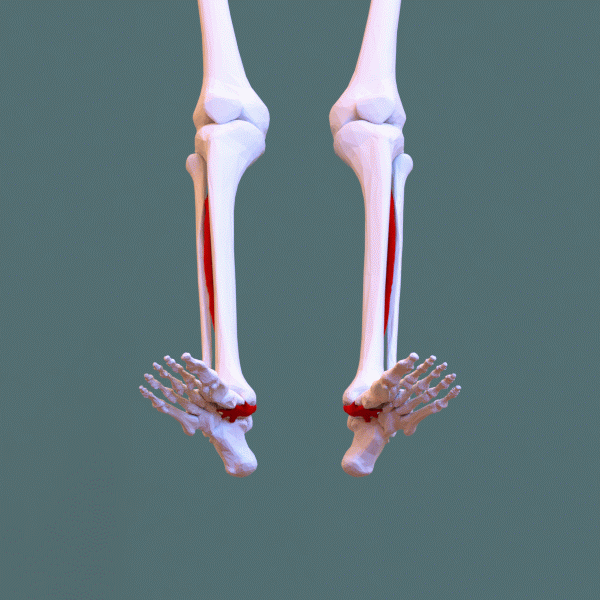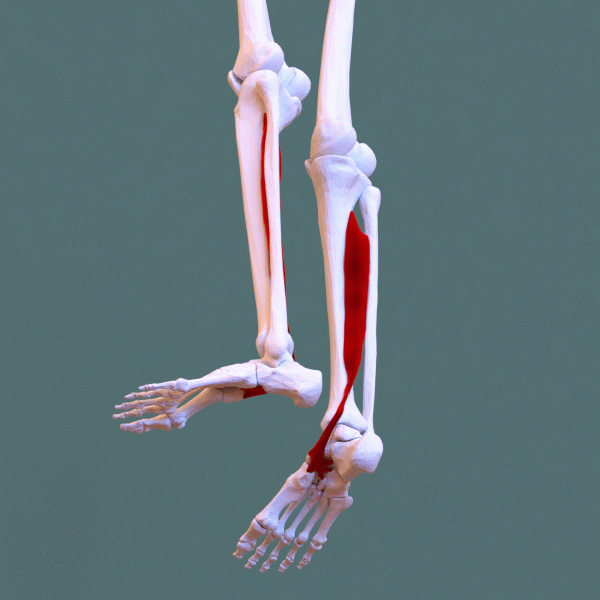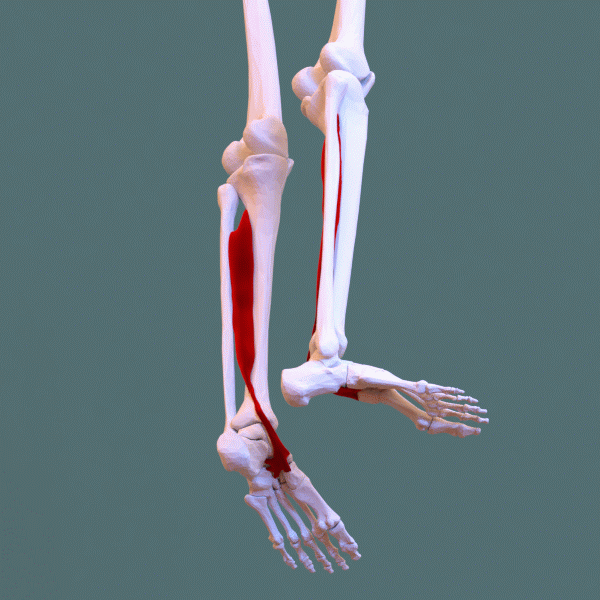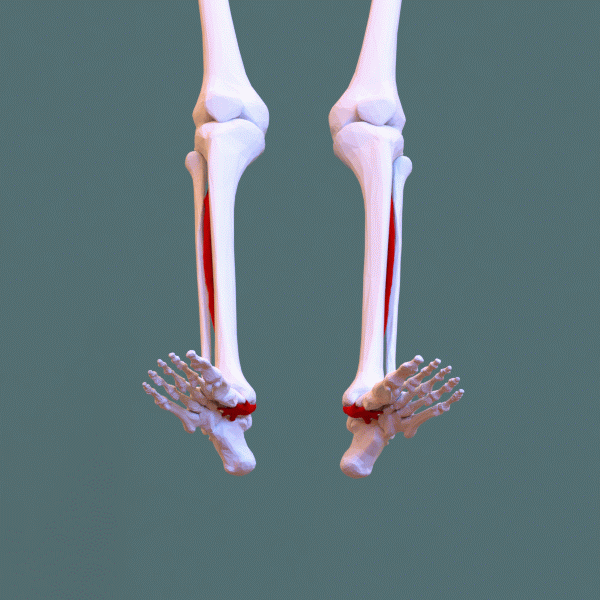
Posterior tibial tendon dysfunction (PTTD) — also called adult-acquired flatfoot deformity (AAFD) — is the progressive failure of the posterior tibial tendon, which is the primary dynamic stabilizer of the medial arch. As the tendon weakens, stretches, and eventually ruptures, the medial arch collapses, the heel drifts into valgus, and the forefoot abducts — the classic "too many toes" sign on viewing the foot from behind.
It is most common in women over 40, people with obesity, hypertension, or diabetes, and those who stand on hard surfaces for long periods.
Diagnosis
exam first, imaging secondThe single-leg heel rise test — inability to rise onto tiptoe on the affected side — is the key exam finding (the tibialis posterior inverts the heel during heel rise). Weight-bearing AP, lateral, and hindfoot alignment X-rays quantify arch collapse and heel valgus. MRI stages tendon degeneration. The Johnson-Strom / Myerson classification (stages I–IV) guides treatment.
Treatment Path
how care progresses at OSIAnkle-foot orthosis (AFO) / custom orthotic
UCBL orthosis (for early stages) or rigid AFO controls hindfoot valgus and supports the arch.
Physical therapy
Tibialis posterior eccentric strengthening and calf stretching.
Activity modification
Reducing impact and prolonged standing.
Surgical Options at OSI
if non-operative care isn't enoughStages I–II with failed conservative management and stages III–IV typically require surgical correction.
Further Reading
authoritative sourcesExternal patient-education references and related OSI pages for additional background:
