Overview
what it is and why it matters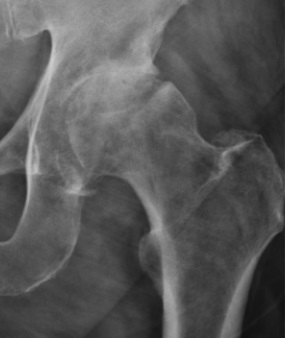
Hip osteoarthritis is the slow wearing-out of the cartilage that lines the ball-and-socket joint of the hip — the rounded head of the femur and the matching surface of the acetabulum, the socket in the pelvis. Cartilage is a smooth, almost frictionless tissue, but it has no blood supply and cannot repair itself. Once it thins, the bone underneath begins to carry more load than it was designed for, inflammation sets in, and the joint margins grow small bone spurs called osteophytes. The practical experience is groin or front-of-thigh pain that becomes stiffer with rest and achier with use.
Most hip osteoarthritis is primary — the cumulative product of time, genetics, and body weight. Secondary osteoarthritis follows an earlier event: childhood hip disorders such as developmental dysplasia, Legg-Calvé-Perthes disease, or a slipped growth plate; a fracture that entered the joint; avascular necrosis, in which a segment of bone loses its blood supply; or untreated femoroacetabular impingement. Every pound of body weight translates to roughly three pounds of force across the hip while walking, which is why weight and cartilage health are tightly linked.
Anatomy & Mechanism
why the joint wearsThe hip is a ball-and-socket joint. The femoral head sits deep within the acetabulum, stabilized by the acetabular labrum (a fibrocartilaginous rim), the hip capsule, and surrounding ligaments. Articular cartilage is avascular and has minimal capacity to heal. In OA, chondrocyte homeostasis tips toward breakdown: proteoglycans are lost, collagen becomes fibrillated, and the cartilage progressively thins. Mechanical overload from obesity, residual childhood deformity, or prior trauma accelerates the process; synovial inflammation amplifies pain out of proportion to radiographic severity.
Symptoms
what patients describe- Groin or front-of-thigh pain — the most common presentation; some patients also feel lateral hip or buttock pain
- Morning stiffness that improves within 30 minutes of moving, then recurs after prolonged sitting
- Startup pain with the first steps after rising, briefly improving before returning with extended walking
- Loss of range of motion, most noticeable when putting on shoes and socks, crossing legs, or getting in and out of a car
- Night pain and intolerance of sleeping on the affected side as the disease progresses
Diagnosis
exam first, imaging secondThe diagnosis is clinical and radiographic. On examination, loss of internal rotation with the hip flexed to 90° is the most sensitive finding; the FADIR test (flexion–adduction–internal rotation) and log-roll test reproduce groin pain. Weight-bearing anteroposterior pelvis and lateral hip X-rays show the four classic features: joint-space narrowing, subchondral sclerosis, subchondral cysts, and marginal osteophytes (Kellgren-Lawrence grading). Non-weight-bearing films systematically underestimate cartilage loss.
MRI is not required for typical OA and is reserved for suspicion of avascular necrosis, occult fracture, or a labral problem in a younger patient. Laboratory testing is indicated only when inflammatory or crystalline arthritis is on the differential.
Nonoperative Treatment
first line for most patientsThe first goal of treatment is to make the hip comfortable enough to keep using it. A stepwise plan built on exercise, weight management, and oral analgesics relieves symptoms for many patients and delays — sometimes indefinitely — the need for surgery.
Activity modification & weight loss
Joint forces at the hip reach three to six times body weight while walking. Cycling, swimming, and elliptical work preserve cardiovascular fitness without concentrating load on the joint.
Supervised physical therapy
Strong hip abductors — the muscles on the side of the pelvis — steady the pelvis during each step and reduce the force the cartilage has to absorb. Core strengthening and targeted manual therapy round out the program.
Oral and topical analgesics
Acetaminophen offers modest relief. Anti-inflammatory medications (ibuprofen, naproxen, meloxicam) provide greater pain control when heart, stomach, and kidney health allow. Topical diclofenac applied to the skin is an alternative when oral anti-inflammatories are not a safe option.
Cortisone injection
A cortisone injection placed in the hip joint under fluoroscopic or ultrasound guidance can provide weeks to several months of relief and is useful as a bridge to therapy gains or a planned surgery. It is not a durable solution; repeated frequent injections are avoided.
Assistive devices
A cane held in the hand opposite the painful hip unloads the joint by up to 25% and often allows longer, more comfortable walking.
Biologic injections (PRP)
Platelet-rich plasma is prepared from your own blood and injected into the joint. Evidence in the hip is limited, and it is considered only in selected patients after standard options have been tried. PRP is not covered by insurance and is offered at a flat self-pay rate.
Operative Treatment
when function no longer respondsSurgery is considered when nonoperative care is no longer sufficient — pain limits sleep, daily activities, or work; medication dependence is increasing; or function has declined despite structured therapy. Total hip replacement is among the most successful operations in medicine, with more than 95% of implants still in place and working well a decade after surgery.
Primary procedure
Posterior total hip replacement
The most widely performed approach. Excellent long-term durability with a familiar, reproducible technique.
Learn about this procedure →Additional option
Anterior total hip replacement
Muscle-sparing interval between sartorius and tensor fasciae latae. Faster early recovery in many patients; long-term outcomes equivalent to the posterior approach.
Learn about this procedure →Recovery & Expectations
what care looks like after surgeryRecovery after hip replacement moves through predictable phases, but the pace is individual. Early on, the focus is on walking short distances, managing swelling, and regaining hip motion with an assistive device. The middle phase adds strengthening — particularly the hip abductors — and weans the assistive device as balance and gait normalize. The final phase is a gradual return to everyday activity and low-impact recreation once pain and strength allow.
Return to driving, desk work, and physical labor is determined by the patient’s progress, not by a calendar. Venous thromboembolism prophylaxis is standard after hip arthroplasty. Your OSI provider sets activity targets at each visit based on what your hip is actually ready for.
When to Contact Us
making the callSchedule an evaluation for groin or hip pain that has persisted beyond six weeks, limits activities you value, wakes you at night, or no longer responds to over-the-counter medication. Call sooner for a sudden inability to bear weight, fever with joint pain, or pain after a fall.
Providers Who Treat Hip Osteoarthritis
joint-replacement teamDavid B. Templin, M.D.
Trent Twitero, M.D.
Further Reading
authoritative sourcesExternal patient-education references and related OSI pages for additional background:



